Allergen immunotherapy in practice: a refresher

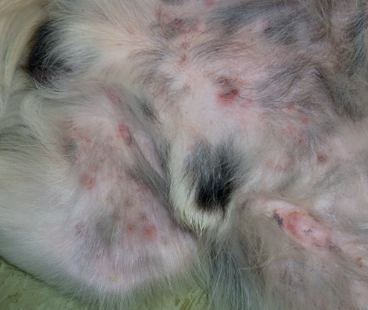
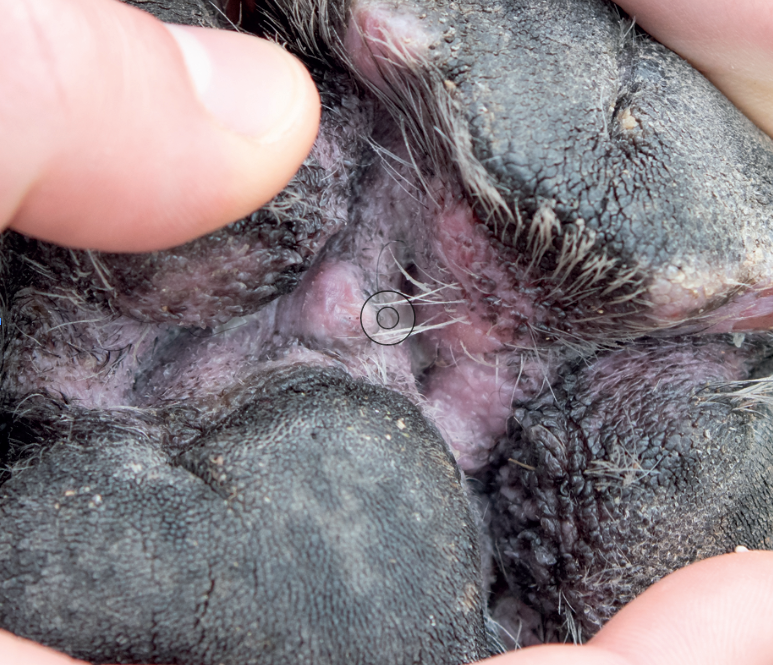
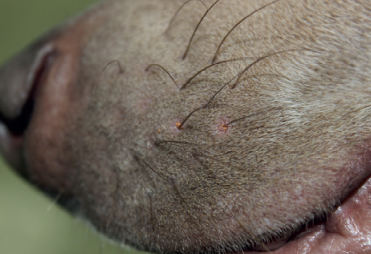
Atopic dermatitis (AD) is a genetically-predisposed inflammatory and pruritic skin disease with characteristic clinical features that is associated with IgE antibodies, most commonly directed against environmental allergens. Canine AD is a common chronic disease that requires a multimodal approach for successful treatment, says Kathryn Cuddy.
Diagnosis
A definitive diagnosis of canine AD can be difficult due to the diversity of the clinical presentation, which depends on genetic factors, the extent of the lesions, and the presence of secondary infections or other flare factors. Hensel et al (2015) have published a set of practical guidelines that can be used to assist practitioners in the diagnosis of canine AD.
Treatment options
ICADA (International Committee on Allergic Diseases of Animals) published consensus guidelines for the treatment of canine AD in 2010, and a minor update in 2015. A complete rewrite is due in 2020. AIT is recommended as a treatment option to prevent recurrence of signs of chronic canine AD. AIT and proactive intermittent topical glucocorticoid applications are the only interventions likely to prevent or delay the recurrence of flares of AD.
Mechanism of action of AIT
The exact mechanism of action of AIT is not fully understood. Mueller et al (2018) recently described how the early response is attributed to reduction in effector cell activity, followed by a long-term immunologic shift from a Th2- to Th1-biased response and development of immunologic tolerance. The shift to Th1 is accompanied by an increase in T-regulatory cells and IL-10 during successful AIT.
Allergy testing
Both intradermal and serum allergy testing are available. The diagnosis of canine AD is based on signalment, history and clinical signs. The aim of testing is to identify allergens suitable for AIT in animals that have been diagnosed with atopic dermatitis. There are patients with canine AD for which no allergen-specific IgE can be detected with either form of testing, and allergen-specific IgE may be detected in healthy dogs. These tests, therefore, cannot be used to make a diagnosis of canine AD. The success rates of AIT with either testing method seem to be the same.
Withdrawal times for any concurrent medications must be observed before testing. Practitioners should consult their serum allergy testing laboratory for their recommendations, as there are slight differences between laboratories.
Testing can be performed at any age. The ideal time is when the patient has been exposed to all allergens that are likely to cause a problem, and has a fully mature immune system. Re-testing may be indicated if the animal moves to a different location, if the seasonal pattern of disease changes, or if the animal was less than 12 months of age when first tested.
Selection of relevant allergens
The results of allergy testing should be interpreted alongside the patient’s clinical history in order to determine if the patient is exposed to the allergen(s) it has reacted to. Interpretation can be challenging, however, and data on the major allergens relevant for dogs is limited. A 2016 position paper by Mueller et al. summarised the current knowledge:
• Dust mites are considered to be relevant and important allergens. Dermatophygoides pteronyssinus is the predominant dust mite in the UK. The clinical relevance of storage mite sensitivity is less clear. Prominent cross-reactivity has been reported between house dust and storage mite antigens in the dog that can explain false-positive results.
• Cross-reactivity has also been demonstrated in the tree, grass and weed pollen groups. Concurrent positive reactions among botanically closely-related plant allergens were significantly more common than those among nonrelated allergens.
• Flea allergy is one of the most common allergies in the dog, and other insect allergies are relatively rare.
AIT formulations
Subcutaneous and oral formulations of AIT are commercially available. The success rates of both formulations are similar. Intra-lymphatic AIT is an exciting area of research.
Subcutaneous immunotherapy (SCIT)
Treatment consists of administering gradually increasing quantities of allergen extract by subcutaneous injection. The frequency of injection depends on whether aqueous or alum-precipitated extracts are used. The injections are administered over an induction period until a maintenance dose is reached. Commercially-available AIT is supplied with a recommended dosage and frequency schedule.
The standard induction protocol consists of administering a slowly increasing concentration of allergen extract over a time period of several months. The rush induction protocol consists of administering a rapidly increasing concentration of allergen extract over a time period of several hours. Rush protocols in humans are associated with a relatively high incidence of systemic reactions; in veterinary medicine, there is no increase in frequency of side-effects compared to the standard protocol. The main advantage of the rush protocol is convenience; it will not affect the rate or speed of response. The rush protocol should be performed in a hospital where the animal can be intensively monitored by experienced clinicians.
The maintenance dose is administered typically every four weeks. The amount of allergen and the frequency of injections should be tailored to the individual patient. If the patient is consistently pruritic following injection, the dose should be reduced. If the patient consistently becomes pruritic before the next injection is due, the frequency should be increased. The patient may benefit from more frequent injections during times of peak allergen exposure.
Oral immunotherapy (OIT)
Treatment consists of administering allergen solution between the lips and gums once to twice daily. Dogs should not eat or drink for 10 minutes before or after administration. Reasons to select OIT over SCIT include owner preference, for dogs who are difficult to inject or which have experienced an adverse reaction to injection, or for dogs which have failed to respond to SCIT.
Concurrent treatment
Many patients will require additional antipruritic therapy during the first few months of AIT, but glucocorticoids and other immunosuppressive therapies may affect the mechanism of AIT. Lokivetmab, essential fatty acids, antihistamines and topical therapies are unlikely to interfere with tolerance induction. Many dermatologists prefer to avoid glucocorticoids, ciclosporin and oclacitinib as long-term therapy during the first year of AIT, but rather as short treatment courses as needed. Topical glucocorticoids are preferred over systemic.
Efficacy of AIT
The full response to treatment cannot be measured until 12 months after commencing AIT. Success rates vary, but in most studies approximately two-thirds of the dogs show a good-to-excellent response. A suggested benchmark for success is at least a 50 per cent improvement in clinical signs and/or pruritus, or at least a 50 per cent reduction in anti-inflammatory treatment requirements. The presence of chronic secondary skin changes will worsen the prognosis.
AIT is usually lifelong. In dogs exhibiting a prolonged complete remission of signs, the frequency of administration should be slowly decreased and eventually stopped, and they may have sustained benefit for months to years.
Adverse effects
AIT is an extremely safe form of treatment, and adverse effects are uncommon. The most common adverse effect is an increase in pruritus after SCIT. The dose of immunotherapy should be reduced if this happens consistently. Injection site reactions such as a localised swelling may occur in some patients. Systemic reactions occur in less than one per cent of patients, and include urticarial, angioedema, GI disturbances, behavioural changes, weakness, and very rarely, collapse and anaphylaxis.
Contraindications
AIT is contraindicated in diseases that affect the immune system, including immunodeficiency, malignant disease and autoimmune disease. It is also contraindicated with renal disease, or if the patient is unwell or pyrexic. AIT cannot be recommended for pregnant and lactating animals as safety studies have not been performed. AIT should not be administered at the same time as vaccinations; at least one week is recommended between injections.
Summary
AIT is the only specific therapy for canine AD, and the only treatment that can modify the patho-mechanisms of the disease. It is a safe, efficacious and cost-effective therapy that remains a cornerstone in the treatment of canine AD.
Kathryn Cuddy MVB CertAVP(VD) MRCVS is an RCVS advanced practitioner in veterinary dermatology. She established Skinvet Ireland in 2015, and opened a dedicated dermatology referral clinic in Midleton, Co. Cork, in 2019.
References and recommended reading
Buckley L, Schmidt V, McEwan N et al; Cross-reaction and co-sensitization among related and unrelated allergens in canine intradermal tests. Veterinary Dermatology 2013;24:422-e92.
Gedon NKY & Mueller RS. Atopic dermatitis in cats and dogs: a difficult disease for animals and owners. Clin Transl Allergy 2018;8:41.
Hensel P, Santoro D, Favrot C et al. Canine atopic dermatitis: detailed guidelines for diagnosis and allergen identification. BMC Veterinary Research 2015;11:196.
Loewenstein C & Mueller RS. A review of allergen-specific immunotherapy in human and veterinary medicine. Veterinary Dermatology 2009; 20(2): 84-98.
Mueller RS, Janda J, Jensen-Jarolim E et al. Allergens in veterinary medicine. Allergy 2016;71:27-35.
Mueller RS, Jensen-Jarolim E, Roth-Walter F et al. Allergen immunotherapy in people, dogs cats and horses – differences, similarities and research needs. Allergy 2018;73:1989-1999.
Mueller RS. Update on allergen immunotherapy. Vet Clin Small Anim 2019;49:1-7.
Olivry T, DeBoer J, Favrot C et al. Treatment of canine atopic dermatitis: 2010 clinical practice guidelines from the International Task Force on Canine Atopic Dermatitis. Veterinary Dermatology 2010;21:233-248.
Olivry T, DeBoer DJ, Favrot C et al. Treatment of canine atopic dermatitis: 2015 updated guidelines from the International Committee on Allergic Diseases of Animals (ICADA). BMC Veterinary Research 2015;11:210.